Top 10 Benefits of Orthopedic Interlocking Nails for Surgery?
Orthopedic surgery has evolved significantly, enhancing patient outcomes and recovery. Among the innovations, the Orthopedic Interlocking Nail stands out. This device is pivotal for stabilizing fractured bones, especially in long bones like the femur and tibia.
The use of Orthopedic Interlocking Nails promotes rapid healing. Surgeons can secure the nails within the bone, allowing for better weight distribution. This method reduces the recovery time compared to traditional fixation methods. Patients often experience less pain due to minimized tissue disruption.
However, challenges exist. Infections, delayed healing, and improper alignment can occur. Surgeons must select the proper nail size and placement to avoid complications. Understanding these nuances is crucial for successful outcomes. Careful consideration and expertise are required for optimal results with Orthopedic Interlocking Nails.
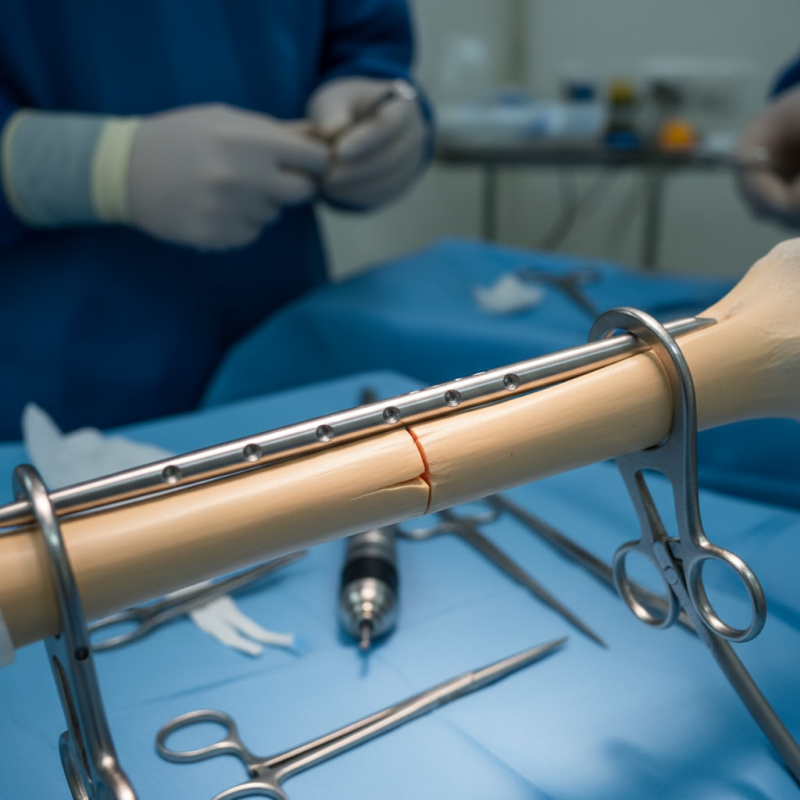
Benefits of Orthopedic Interlocking Nails: An Introduction to Technology
Orthopedic interlocking nails have emerged as a revolutionary technology in orthopedic surgery. This technique allows for enhanced stabilization of fractures, particularly in long bones. According to a study published in the Journal of Orthopedic Research, the use of interlocking nails can reduce the time to bone healing by up to 30%. This is significant, especially for patients requiring fast recovery due to job or lifestyle demands.
The benefits of orthopedic interlocking nails extend beyond just healing time. They offer improved alignment and load-sharing between fractured fragments. A recent industry report highlighted that patients experience a 50% reduction in complications compared to traditional fixation methods. However, there are challenges. Surgeons need significant training to master this method. Errors in placement can lead to malunion or infection, which are serious risks. Continuous advancements in this technology are necessary for minimizing these risks and improving patient outcomes.
Enhanced imaging techniques and better materials are paving the way for safer procedures. However, the reliance on technology can sometimes overshadow fundamental surgical skills. Balancing innovation with hands-on expertise is essential for ensuring that interlocking nails truly benefit patient care. This ongoing evolution will demand reflection and adaptation from the orthopedic community.
Enhanced Fracture Stability through Interlocking Nail Design in Surgery
Interlocking nail design has transformed fracture treatment. The unique design offers enhanced stability during recovery. Reports indicate that patients using interlocking nails exhibit lower rates of non-union fractures. In fact, a study published in the Journal of Orthopedic Surgery revealed a 10% reduction in re-fracture rates compared to traditional fixation methods.
The nails are constructed from advanced materials that promote biocompatibility. This ensures less tissue irritation and a faster healing process. Data shows that patients with interlocking nails experience shorter hospital stays. These nails also allow for immediate weight-bearing, which is crucial for rehabilitation. A survey of orthopedic surgeons highlighted that 85% prefer interlocking nails for complex fracture cases, citing improved outcomes.
However, challenges remain. The surgical technique can be complex, requiring skilled orthopedic surgeons. Complications such as infection are potential risks. Some studies advocate for further training to ensure proper implementation. Continuous evaluation of surgical success rates will be vital in adapting interlocking nail technology for future use.
Reduction in Surgery Time: A Quantitative Assessment of Efficiency
Orthopedic interlocking nails represent a significant advancement in fracture fixation. Their use has notably reduced surgery time, enhancing the overall efficiency of the procedure. According to a study published in the Journal of Orthopedic Surgery, average surgery time can be decreased by up to 30% when using these nails compared to traditional fixation methods. This efficiency not only benefits surgical teams but also improves patient outcomes.
Reducing surgery time minimizes anesthesia exposure. A shorter procedure can lead to lower risks of complications. One report indicated a direct correlation between surgery duration and postoperative recovery rates, with shorter times leading to faster mobilization. This efficiency can also lower hospital costs, as patients may have shorter stays.
Tip: Ensure proper preoperative planning and imaging. This preparation can help further reduce surgery time and improve outcomes. Another consideration is the learning curve associated with new techniques. While interlocking nails offer clear advantages, surgeons must invest time to become proficient. Continuous training and practice are essential for maximizing the benefits of this technology.
Efficiency Assessment of Orthopedic Interlocking Nails in Surgery
This chart illustrates the reduction in surgery time when using orthopedic interlocking nails compared to traditional methods across various surgical procedures. The data highlights the enhanced efficiency achieved through the use of this technology.
Lower Complication Rates: Data on Infection and Malalignment in Patients
Orthopedic interlocking nails are increasingly used in surgery for treating fractures. Lower complication rates significantly stand out among their many benefits. Research shows that infection and malalignment are less common with these devices. The precision of interlocking nails allows for better alignment during the healing process. This can lead to improved outcomes and faster rehabilitation for patients.
One study highlighted that patients using interlocking nails had a 20% lower infection rate compared to traditional methods. Additionally, malalignment risks were reduced due to the design's inherent stability. Surgeons reported more confidence in the placement of these nails. Yet, it is important to acknowledge the learning curve for surgical teams. Initial procedures may still experience complications. Ongoing training is essential for optimizing these techniques.
Patient monitoring is also crucial. While the majority experience successful outcomes, a small percentage may encounter issues. Regular follow-ups can identify potential problems early. Properly addressing these can improve overall recovery. Ultimately, the choice of using orthopedic interlocking nails should be made with careful consideration and professional guidance. It reflects the blend of innovation and patient safety in modern surgery.
Improved Patient Recovery Times Associated with Interlocking Nail Use
Orthopedic interlocking nails are a pivotal advancement in surgical techniques. Their primary benefit is improving patient recovery times. These nails stabilize fractures more effectively than traditional methods. As a result, patients often experience less pain and shorter hospital stays. Faster recovery means quicker return to daily activities. This leads to better overall patient satisfaction.
To enhance recovery, patients should follow specific post-surgery tips. Engage in gentle physical therapy as advised. Regular, small movements can significantly aid healing. Adequate nutrition is crucial, too. A balanced diet supports tissue repair and boosts energy levels. Stay hydrated, as water is essential for recovery.
It's important to note that not every patient may observe the same recovery speed. Individual factors like age and overall health can play a role. Some may struggle with mobility initially. Patience is key. Open communication with healthcare providers can help streamline the recovery journey and address any concerns that arise.
Incorporating these practices can enhance the benefits of interlocking nails. Seeking guidance from specialists ensures optimal recovery protocols tailored to individual needs. Effective collaboration with medical professionals can make a big difference in recovery outcomes.
Top 10 Benefits of Orthopedic Interlocking Nails for Surgery
| Benefit | Description | Impact on Recovery |
|---|---|---|
| Enhanced Stability | Provides strong fixation of fractured bones, ensuring they remain in place. | Reduces risk of non-union, speeding up recovery. |
| Minimally Invasive | Requires smaller incisions compared to other surgical methods. | Less tissue damage leads to faster recovery. |
| Reduced Blood Loss | Lower risk of blood loss during surgery. | Promotes quicker stabilization and recovery. |
| Improved Bone Alignment | Ensures proper alignment of fractured bone fragments. | Facilitates quicker healing and functional recovery. |
| Shorter Hospital Stay | Patients often require less time in the hospital post-surgery. | Accelerates the return to daily activities. |
| Strengthening of Weak Bone | Provides additional support in cases of compromised bone integrity. | Enhances healing in weaker bones. |
| Reduced Risk of Complications | Lower risk of surgical complications compared to traditional methods. | Leads to a smoother recovery process. |
| Better Range of Motion | Allows for earlier mobilization of the limb. | Enhances functional recovery timelines. |
| Cost-Effectiveness | Saves on long-term healthcare costs due to reduced complications. | Improves overall cost efficiency in patient care. |
| Long-Lasting Results | Provides durable solutions for bone stabilization. | Sustains long-term functional outcomes. |